A RESPONSE TO STATE FINANCIAL OFFICERS’ CALL TO ACTION
State Financial Officers across the United States have formally urged Fortune 500 companies to conduct rigorous payment integrity reviews of their healthcare spending. These officers, acting as fiduciaries for public investment funds, have reframed healthcare overspending from an HR issue to a direct threat to shareholders. Their goal is clear: control costs, mitigate risk, and protect shareholder value.1
SmartLight clients can respond with confidence to the State Financial Officers’ call to action.
THE CASE FOR INDEPENDENT MONITORING
Employer healthcare spending in the United States is projected to reach $1.83 trillion this year. This massive expenditure demands the same financial discipline and independent scrutiny applied to any other major corporate cost.2
The letter from the State Financial Officers implies the conventional approach—relying on carriers, third-party administrators, and pharmacy benefit managers to audit their own billing—is fundamentally flawed.
THE CARRIER CONFLICT OF INTEREST
-
- Revenue Risk: When carriers identify and reimburse plans for overpayments, they often reduce their own revenue streams.
-
- Ineffective Audits: Random, self-directed “spot checks” frequently miss billing anomalies, duplicate payments, deviations from contracted rates, and cannot identify systemic payment errors.
-
- Flawed Incentives: Payment integrity “shared savings” programs are often designed to cost plan sponsors more by paying carriers to fix their own billing mistakes, and plan sponsors are paying twice for services typically included in core administrative services.
These systemic flaws drive up costs and liability for employers, eroding shareholder value.
Independent, continuous oversight is a best practice—and a fiduciary imperative.
THE SMARTLIGHT ANALYTICS APPROACH
SmartLight Analytics partners with the nation’s largest employers to provide continuous, independent claims integrity review and advocacy.
-
- 100% Claims Analysis: SmartLight analyzes every medical, pharmacy, and dental claim on a continuous basis. This eliminates the sampling gaps in traditional audits, preventing small errors from turning into million-dollar losses over time.
-
- Proprietary Detection Systems: The SmartLight platform leverages proprietary models to identify payment anomalies across complex claims datasets.
-
- Clinical and Investigative Validation: Flagged issues are reviewed by clinical and investigative teams that validate accuracy against your specific contracts. SmartLight claims advocates then work directly with carriers to fix root causes, not just isolated incidents.
MEASURABLE FINANCIAL RECOVERY
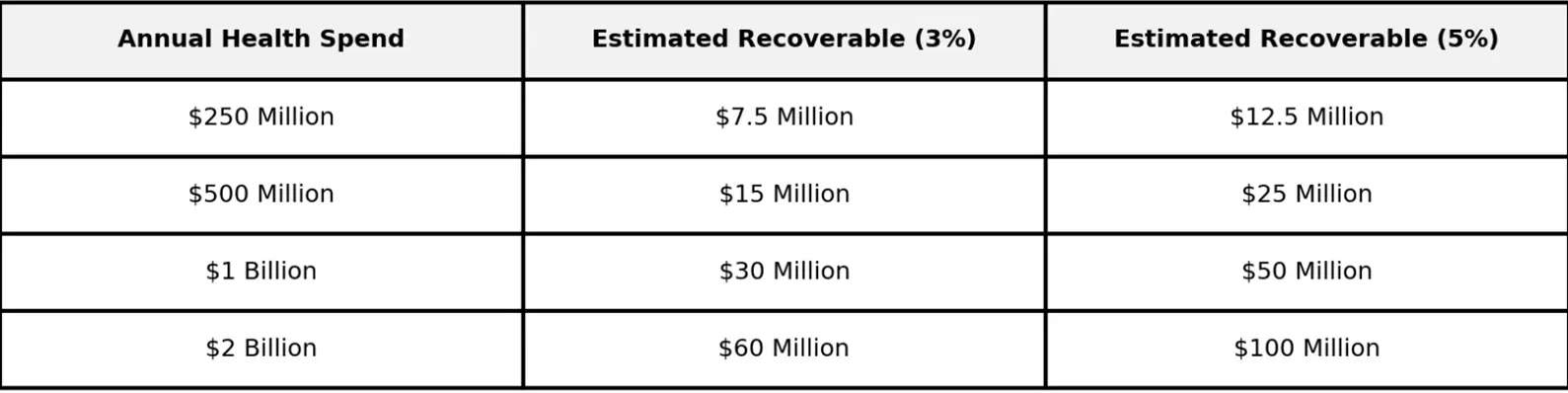
The math is compelling. SmartLight clients consistently recover ~3–5% of total health spending, returning those funds to the bottom line.
THE COST OF INACTION
Organizations that delay face compounding risks: continued overspending and potential regulatory scrutiny. Those that implement independent healthcare expense monitoring now will be better positioned ahead of emerging compliance requirements and are better prepared to defend their fiduciary practices to investors, boards, and regulators.
SmartLight Analytics is your claims integrity advocate, delivering independent analysis, actionable intelligence, and measurable savings.
PROTECT YOUR SHAREHOLDER VALUE TODAY
www.smartlightanalytics.com | info@smartlightanalytics.com
¹ National Association of State Auditors, Comptrollers and Treasurers (NASACT) / State Financial Officers Foundation. Letter to Fortune 500 Chief Financial Officers regarding healthcare payment integrity. December 2024.
² Centers for Medicare & Medicaid Services (CMS). (2026). National Health Expenditure Projections 2024-2033: Forecast Summary. Office of the Actuary.