
Exposing waste in our health care system means taking action now
Seeing health care costs through the lens of data analytics gives employers with self-funded health care plans the view to one way in which the problem can be addressed right now. Eliminating even a portion of the dollars being lost to fraud, waste, and abuse within health care claims would have a substantial impact in lowering per member per month costs for employers. READ MORE>
Smarter methodology goes beyond analytics:
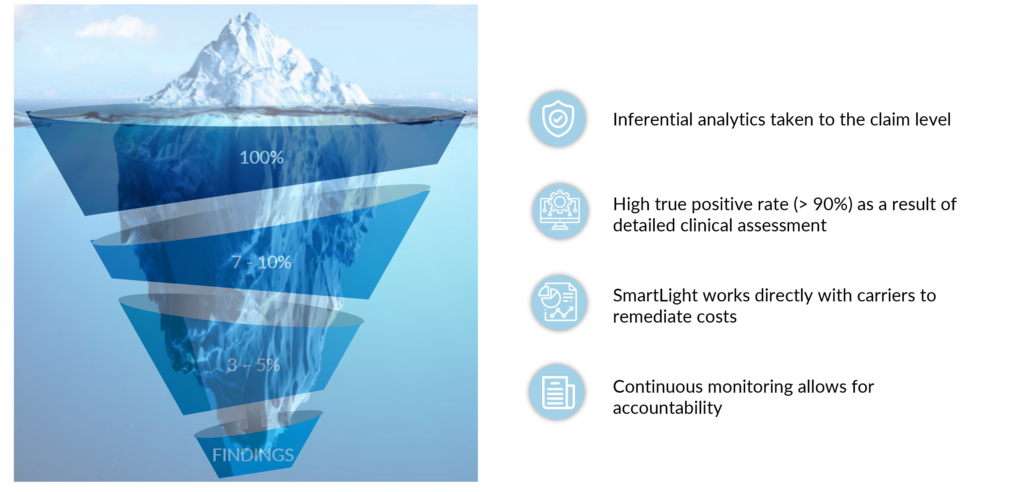
Your data tells us where to look to find outliers and irregular patterns in your claims and our clinical and adjudication experts minimize false positives.
Monthly reviews allow for immediate intervention, leading to substantial savings and refunds applied toward the plan funds.
The Difference
PARTNER WITH SMARTLIGHT
[yikes-mailchimp form="2"]
